


95%
99%
4-5x
Tangible Results For Hospitals & Health Systems







How Our Hospitals & Health Systems IDR Process Works
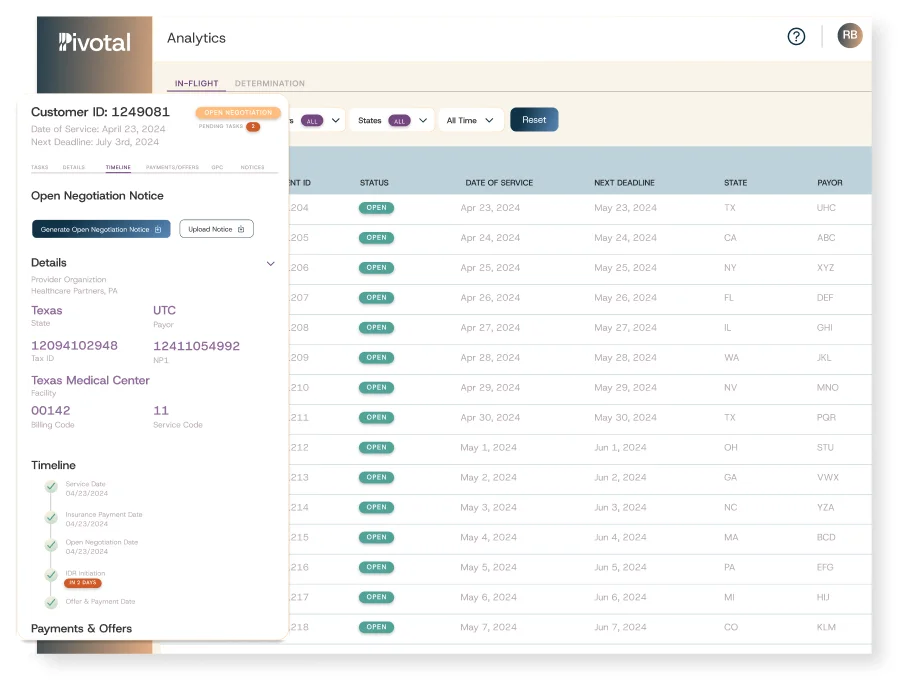
Seamless Integration
Strategic Evaluation
Expert Execution
Superior Results

Emergency Medicine IDR Solution: FAQs

Independent Dispute Resolution (IDR) allows hospitals and health systems to challenge underpaid out-of-network claims under the No Surprises Act. Because hospital claims are high-volume and complex, successful IDR requires scalable workflows, strong documentation, and data-driven strategy.

Hospitals and health systems face increasing reimbursement pressure as payer rates decline under the No Surprises Act. IDR provides a critical mechanism to recover fair payment across large, multi-facility organizations.

Pivotal Health provides a full-service IDR solution designed for enterprise healthcare organizations, combining automation, analytics, and expert support. We help health systems manage high claim volumes efficiently while improving reimbursement outcomes.

Yes, Pivotal Health integrates with hospital revenue cycle management (RCM) systems to streamline data flow and minimize operational disruption, with no IT lift or EHR integration required. This enables health systems to scale IDR without adding internal administrative burden.

Identifying which claims are eligible for IDR can be complex. IDR eligibility is based on factors such as the place of service (ED, inpatient, outpatient hospital ASC), network status, provider specialty, CPT codes, and facility type. It also requires an understanding of whether a claim falls under federal versus applicable state IDR rules. Pivotal Health ingests claims on behalf of hospitals and health systems using a custom eligibility engine, historical claims data, and automation to surface eligible claims.
For health systems committed to fair reimbursement, Pivotal Health's IDR platform recovers your rightful compensation.




Citation: [1] Explainer: Federal independent dispute resolution process for surprise medical bills Citation: [2] EDPMA Data Analysis: No Surprises Act Independent Dispute Resolution Effectiveness